Case Study
Interesting Facts About Radiology
Learn interesting facts about radiology from interesting cases that we encounter at the AMI centers worldwide. Gain insights into how our internationally-acclaimed radiologists diagnose and treat rare conditions. Take a peek into the mysteries of human health, and how our expert teams handle them.
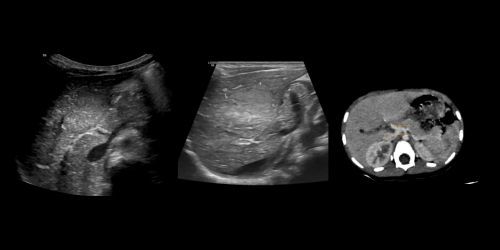
Congenital Extrahepatic Portosystemic Shunt
A 3-year-old male child with h/o of abdominal pain and USG shows hyperechoic area in liver. Findings: 1....
17/11/2023
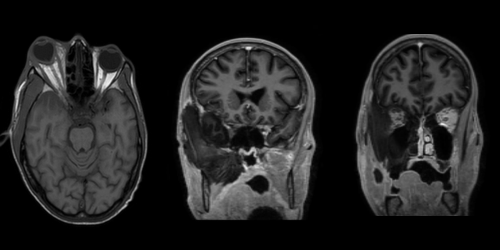
Mucormycosis
• 43 year old, male presented with fever ,cough and breathing difficulty– 1 week &nb...
17/11/2023
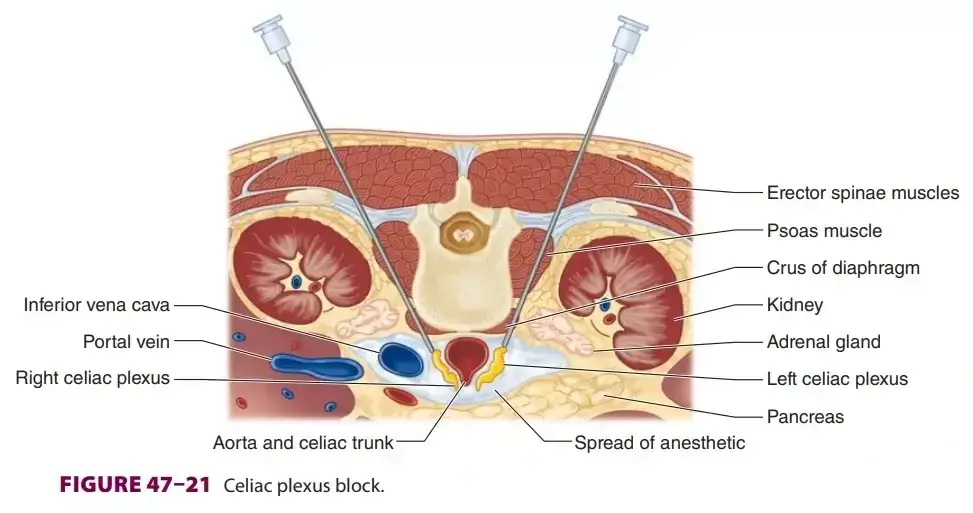
Celiac plexus block
37 year old male present with severe abdominal pain due to chronic pancreatis. Inoperable malignant intraducta...
20/12/2022
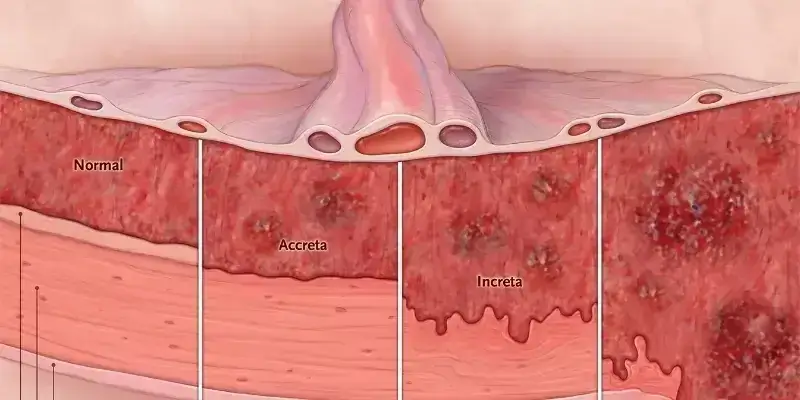
Managing Adherent Placenta – Triple Doctor’s Story.
Adherent Placenta are abnormal placenta leading to severe post-partum haemorrhage. Even by controlled caesarea...
08/12/2022

AMI Expertise - When You Need It, Where You Need It.
Partner With Us
